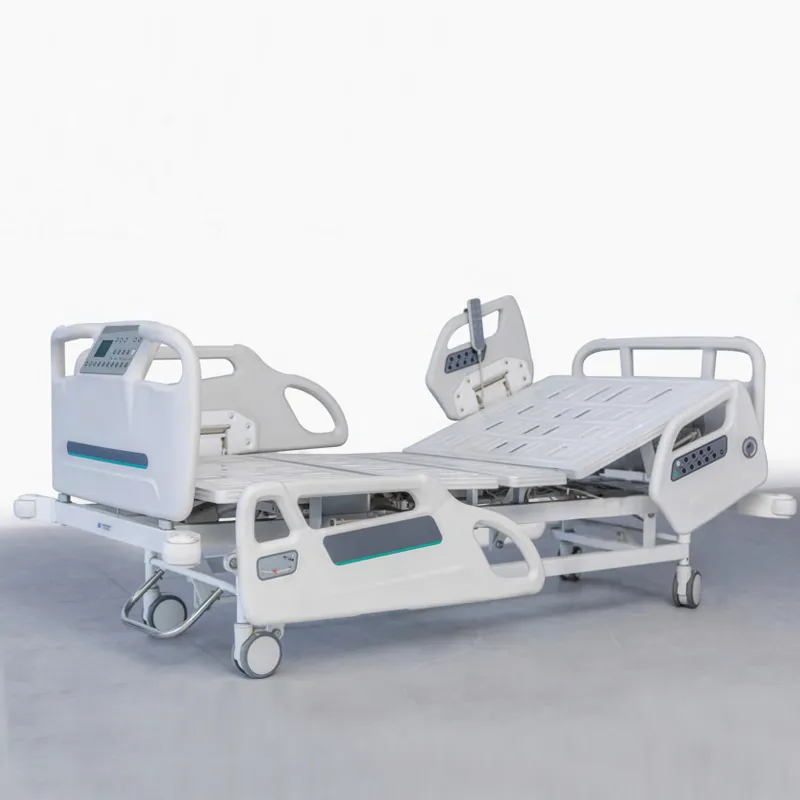
Why Ease of Operation Is Critical for Electric Hospital Beds
How easy electric hospital beds are to operate makes a real difference for both patients and caregivers. People with limited mobility conditions like ALS or Parkinson's benefit greatly from simple control systems that let them adjust their position on their own. According to some rehab research, this independence cuts down fall risks by about a third during bed adjustments. Patients feel more respected when they can move themselves around, plus it helps prevent pressure sores from developing. The benefits extend beyond just the patients too. Nurses and other staff members face significantly less strain on their bodies when working with these beds. A recent study from the Ergonomics Safety Council found that caregivers suffer roughly 41 percent fewer back and muscle injuries when handling electric beds compared to traditional manual models.
In emergencies, straightforward functionality allows rapid bed articulation without cognitive overload. Integrated battery backup systems—essential during power outages—further reinforce reliability. Ultimately, seamless operation bridges clinical outcomes and human-centered design: cutting staff fatigue, accelerating response times, and empowering vulnerable patients through self-managed comfort.
Key Dimensions of Ease of Use in Electric Hospital Bed Controls
Physical Interface Design for Diverse Users
Hospital bed controls need to work for people with all sorts of physical limitations. Big buttons that stand out visually and give feedback when pressed help those who struggle with poor eyesight, shaky hands, or arthritic joints something many seniors and folks with neurological issues deal with daily. The control panel angles are designed so important functions such as stopping emergencies or changing bed height can be reached easily whether someone is sitting up or lying down flat. Surfaces on these controls shouldn't slip around accidentally, and they need to handle constant cleaning without falling apart. We've found that simpler interfaces with fewer buttons cut down mistakes during operation about forty percent better than complicated ones full of options nobody really needs anyway.
Intuitive Control Logic and Low Cognitive Load
Good design really cuts down on how much someone has to think about what they're doing by making things work in ways people expect. Take those single action buttons for basic movements like raising the backrest or adjusting legs - these actually work better than complicated menu systems, particularly when dealing with folks who might struggle with memory issues or concentration problems. Instead of reading words, universal icons show what each button does (like this arrow pointing up means lift, while a square stands for stop). When functions are organized together visually, it just makes everything easier to see at once. The system also gives sounds when something happens so users know their command was received, plus there's an automatic return feature after a set time that stops accidental changes. Medical equipment that only needs one or two steps to make adjustments means patients depend less on caregivers all the time, which is pretty important for maintaining independence.
Reliable Remote Functionality for Patient Independence
Wireless pendants give patients more freedom than just being limited to their bedsides. These devices work reliably on 2.4GHz frequencies, keeping signals strong even when tucked under blankets up to 15 feet away. They last for at least three days on a single charge, and they warn users when power gets low so there are no surprises. The buttons light up at night for easy operation, plus special lock features stop anyone from changing settings accidentally. Hospital staff have noticed something interesting too: when these remote controls function properly and respond quickly, patients ask for help about 30% less often. That means fewer disturbances during rest periods and ultimately reduces the chance of developing those painful pressure sores we all want to avoid.
Real-World Validation: Usability Testing with Clinically Vulnerable Users
ALS and Parkinson’s Patients Using Electric Hospital Beds Independently
Patients with Amyotrophic Lateral Sclerosis (ALS) and Parkinson’s disease face progressive challenges in motor control, making independent equipment use exceptionally difficult. Usability testing with these populations highlights what works—and why:
- High-contrast, large-button interfaces cut errors by 40% among users with tremors
- Sequential control logic (≈3 steps per function) enables 87% of ALS patients to operate beds independently after brief training
- Pendant placement within 15 inches of resting hand position eliminates strain during routine adjustments
According to a recent 2023 rehab study, people with Parkinson's disease were able to make adjustments about 25 percent quicker when they used voice activated systems compared to traditional manual controls. The researchers noticed something interesting too - regardless of which group someone was in, caregivers spent roughly 2 hours and 40 minutes less per day on interventions thanks to these simpler interfaces. When monitored clinically, nearly 8 out of 10 participants who had stage III Parkinson's managed to complete three important tasks all by themselves. These included changing bed heights safely for transfers, getting the Trendelenburg position going, and triggering the emergency flat setting when needed.
This evidence confirms that purposeful control design doesn’t just meet compliance—it transforms electric hospital beds from potential barriers into instruments of dignified, self-directed care.
Industry Standards vs. Practical Accessibility in Electric Hospital Beds
Regulatory standards like ISO 60601-2-52 ensure technical safety—but often miss real-world accessibility gaps. While they specify button force limits (e.g., ≈3.5 newtons), they rarely account for patients whose grip strength falls below 40% of baseline due to rheumatoid arthritis or advanced neurodegeneration. As a result:
- “Certified” interfaces may remain functionally inaccessible to patients with neurodegenerative conditions
- Caregivers frequently override remote features due to confusing menu hierarchies
- Healthcare facilities invest in technically compliant beds that inadvertently erode patient autonomy
True bedside accessibility demands more than checklist compliance. It requires universal design: tactile feedback, voice-activated overrides, and posture-adaptive control placement. Without this shift, standardization risks becoming a façade—one that sustains exclusion rather than enabling inclusion in acute and home-based care settings.